Systemic Fungal Disease – Mycotoxicosis
Ill patients approached us from an evacuated apartment building with several million IAQ counts of toxigenic fungi. These were the highest counts we had ever seen.
In this study, most of whose host defense mechanisms were compromised from toxigenic fungal exposure ranged from minor to fatal and often are caused by organisms that normally reside on or inside body surfaces. In the hospital setting, they frequently result from colonization by antibiotic-resistant organisms (opportunistic fungi) and unskilled physicians who often misdiagnose, disregard, and prescribe drugs that can be potentially detrimental to the immunocompromised hypersensitized patient who often are unknowingly poisoned by the to T-2 mycotoxins from infected buildings.
The American medical industry, who is generally trained in finding a ‘quick fix’ to the immediate symptoms with often ineffective pharmaceuticals, rather than finding a permanent corrective action plan. This generates a great disservice to the general public, who is basically trusting and ignorant to doctors upon their initial consultation, until they discover that these placebo treatments are ineffective and the patient is making no progress; sometimes too late in regards to finding agressive and alternative treatment options for these patients who are at times, gravely ill.
Host defense mechanisms–physiologic, anatomic, or immunologic–may be altered or breached by disease or trauma or by procedures or agents used for diagnosis or therapy. Infections in this setting, often called opportunistic infections, occur if antimicrobial therapy alters the normal relationship between host and microbe or if host defense mechanisms have been altered by age, burns, neoplasms, metabolic disorders, irradiation, foreign bodies, immunosuppressive or cyto toxic drugs, corticosteroids, or diagnostic or therapeutic instrumentation. This ideology has changed over the past five years as patients with normal health histories have incurred systemic fungal infections with exposure to lethal fungi such as stachybotrys and chaetomium causing damage to the myelin sheath. These otherwise normal patients became gravely ill and autoimmune disease was diagnosed within one year to eighteen months on average in 68% of the patients who were exposed to these to fungi types.
In the other patients, systemic fungal disease was diagnosed in 32% with minor symptoms, including reactive airway disease, asthma, GERD, joint/muscle pain, memory problems, balance, vision, and hypersensitivity. Colonization occurred in 46% of these cases and aggressive antifungal protocol had to be followed. All patients followed a rigorous vitamin, enzyme, diet therapy that was highly effective for 97% of all cases when administered in a timely manner.
The underlying alteration predisposes the patient to infections from endogenous micro flora that is nonpathogenic or from ordinarily harmless, saprophytic organisms acquired by contact with other patients, hospital personnel, or equipment. These organisms may be bacteria, fungi, viruses, or other parasites; the precise character of the host’s altered defenses determines which organisms are likely to be involved. These organisms are often resistant to multiple antibiotics, as they contain fungi.
Drug Therapy and Impaired Host Defense Mechanisms
Antibiotics alter the normal micro flora of the skin, mucous membranes, and GI tract and may result in colonization by new organisms. Colonization is harmless unless followed by super infection, which refers to invasion by indigenous or environmental organisms resistant to the administered antibiotic. Factors predisposing to super infection include extremes of age, debilitating diseases, and prolonged treatment with antibiotics, especially broad-spectrum ones. Super infections usually appear on the 4th or 5th day of therapy and may convert a benign, self-limited disease into a serious, prolonged, or even fatal one. The diagnosis of super infection by a normally commensal organism is certain only when the organism is recovered from blood, CSF, or body cavity fluid.
Corticosteroids, often mistakenly prescribed by unskilled or uninformed physicians looking for a ‘quick fix,’ alter many aspects of host defenses; one of the most important is inhibition of the movement of neutrophils, monocytes, and lymphocytes into the inflammatory exudate. Corticosteroids may reactivate quiescent pulmonary TB, histoplasmosis, coccidioidomycosis, and blastomycosis. Patients receiving corticosteroid treatment (especially in high dose) for RA, ulcerative colitis, asthma, sarcoidosis, SLE, pemphigus, or Cushing’s syndrome have increased susceptibility to infection from usual and unusual bacteria and tend to develop infections with chaetomium and stachybotrys, as previously mentioned.
Nosocomial (Hospital-Acquired) Infections
These infections are acquired from the hospital environment or personnel (eg, inadequately sterilized equipment or insufficient hand washing). They usually occur when a susceptible patient has a portal for infection from altered anatomic barriers (see below) or has been given broad-spectrum antibiotics. They are commonly due to Staphylococcus, Enterobacter, Klebsiella, Serratia, Pseudomonas, Proteus, Acinetobacter, Aspergillus, or Candida.
Alterations of Anatomic Barriers
Patients with extensive burns or those undergoing diagnostic or therapeutic procedures that breach normal anatomic barriers to infection (eg, tracheostomy, inhalation therapy, urinary tract instrumentation, indwelling urethral or IV catheter placement, surgery, and surgical prostheses application) are vulnerable to infection by endogenous or exogenous antibiotic-resistant organisms. Gram-negative bacteria, particularly Pseudomonas and Serratia, and other multiply resistant organisms, alone or in combination with staphylococci, cause soft tissue infections and bacteremia in severely burned patients. Significant bacteriuria develops in patients with indwelling urethral catheters, increasing the risk of cystitis, pyelonephritis, and bacteremia with gram-negative bacilli. Sepsis from IV catheter sites, due to staphylococci, gram-negative bacilli, or Candida, may cause local suppuration or severe and sometimes fatal systemic infections. Patients with endotracheal tubes or tracheostomies and others who require repeated tracheal suctioning or inhalation therapy with equipment containing a reservoir of nebulization fluid may develop bronchopulmonary infection, usually with nosocomial gram-negative organisms.
Impaired Cellular or Humoral Host Defense Mechanisms
Neoplastic and immunodeficiency diseases such as leukemia, aplastic anemia, Hodgkin’s disease, myeloma, and HIV infection are characterized by selective defects in host resistance. Patients with hypogammaglobulinemia, myeloma, macroglobulinemia, or chronic lymphocytic leukemia tend to have deficient humoral immune mechanisms and to develop pneumococcal and Haemophilus pneumonia (see also Pneumonia in the Compromised Host in Ch. 73) and bacteremia.
Patients with neutropenia due to leukemia, intensive immunosuppressive therapy, or irradiation frequently develop gram-negative bacteremia from infections acquired through the mucous membranes or secondary to pneumonia (see Ch. 135). Severely immunosuppressed patients and those with Hodgkin’s disease and HIV tend to have depressed cellular immune mechanisms; serious infections with mycobacteria, Aspergillus, Candida, Cryptococcus, Histoplasma, Mucor, Nocardia, or Staphylococcus are frequent. Herpes zoster, cytomegalovirus, Pneumocystis, and Toxoplasma infections also occur. AIDS often leads to infections caused by atypical mycobacteria, herpes simplex, Giardia, Cryptosporidia, Isospora, and many others.
Prophylaxis
Awareness of the patterns of infection that occur in the compromised host helps in early recognition of infections and initiation of appropriate therapy. Awareness of the specific site of breached defense, the type of defense system that has been weakened or lost, and the characteristics of organisms prevalent in a particular institution, based on continuous hospital surveillance, is also helpful.
Antibiotic prophylaxis is indicated for some conditions, including rheumatic fever and bacterial endocarditis, TB exposure, recurrent UTIs and otitis media, bacterial infections in granulocytopenic patients, and some types of Neisseria infections. Prophylaxis with antibiotics is also indicated after vaginal or abdominal hysterectomy; colonic, rectal, cardiac, joint, or vascular surgery; prostatectomy in patients with previous UTIs; and pneumocystis in AIDS patients. However, use of broad-spectrum antibiotics, massive doses of any antibiotic, or prophylactic use of systemic antibiotics may ultimately result in infection with resistant bacteria. Patients receiving antibiotics should be watched for signs of superinfection.
Barriers help control and prevent infection. Strict asepsis should be maintained in diagnostic and therapeutic manipulative procedures. Attendants should wear sterile gloves during endotracheal or tracheostomy suctioning, and suction catheters should be sterile, disposable, and used only once. Masks, tubing, nebulizer jars, and other respiratory therapy equipment connected directly to a patient’s airway should be sterilized by steam or gas before use and should be changed daily. When steam or gas sterilization is not possible, the equipment should be disinfected with a 2% glutaraldehyde or 2% acetic acid wash, followed by thorough rinsing and drying. Alternatively, nebulization of 0.25% acetic acid through the equipment, followed by thorough rinsing, is usually satisfactory for daily cleaning of a ventilator that is in use. Care should be taken to ensure that the gas jets have been completely cleaned.
Urethral catheters must be connected to closed sterile drainage bags and the system kept closed. IV catheters should be inserted securely, covered with a sterile protective dressing, and removed after 48 to 72 h or at the first sign of phlebitis. An ointment of neomycin, polymyxin B, and bacitracin or an iodine ointment (eg, povidone-iodine), applied daily to the cannulation site and the emerging catheter, may help prevent infection. Thrombophlebitis usually responds to catheter withdrawal and local application of hot compresses, but antibiotic therapy for specifically identified or presumed causative organisms may be necessary.
Treatment
Opportunistic infections are difficult to treat once established because the organisms tend to be resistant to most commonly used antibiotics. Short-term therapy tends to merely suppress infection temporarily unless the underlying condition can be corrected (e.g., urethral or IV catheters removed or tracheotomy closed); thus, treatment often must be longer than usual. Cultures and possibly tissue biopsy should be performed before starting or altering antibiotics, but therapy may need to be started while awaiting laboratory results on the basis of clinical-bacteriologic diagnosis and knowledge of the organisms known to be prevalent in a particular institution and their presumptive sensitivity. If possible, corticosteroid dosage and immunosuppressive chemotherapy should be reduced while treating opportunistic infections.
Aggressive treatment is necessary to end mycotoxicosis. There is not a drug available to cure the problem but many help. Antifungals are much more beneficial than cholestyramine. If one wants to create anoxynase in the body, there are far more healthier and economical ways to do it than administering harsh chemicals in the body. There is currently a vitamin/enzyme/mineral/electrolyte therapy that is very helpful but has not been mage available for clinical trial yet. It will soon be available. There are many treatment options available on this website that is approved and very beneficial, and at no charge from us. More updates will be published soon.
NOTE: This is an excerpt from the Finnish Journal of Environmental Medicine – Establishing effective protocols for systemic fungal disease; especially in North American patients.


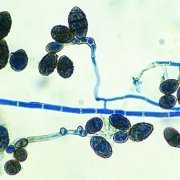 ©Mycology Online, University of Adelaide
©Mycology Online, University of Adelaide 



