The Unexpected and Troubling Rise of Candida auris
Editorial Note:
This article was written by Tom Chiller, MD, chief of the Mycotic Diseases Brand of the CDC, in August 2017. He raised an alarm about Candida auris before it was even fully recognized as a pending epidemic. He commented in a CDC Expert Commentary Series on Medscape, “I would like to tell you about Candida auris, a novel yeast that is behaving in unexpected and concerning ways, causing severe disease in countries across the globe, including the United States.”
He goes on to share: “C auris is quickly becoming more common. In some international healthcare facilities, it has gone from an unknown pathogen to a cause of 40% of invasive Candida infections within a few years. We need to act now to prevent this from happening in the United States.”
His video shows healthcare professionals how they can protect their patients from this “potentially deadly infection, the history of this unusual bug, and how the United States is working with global partners to combat its spread”.
Chiller’s Synopsis of C auris
Several features set C auris apart from other Candida species and make it a particular concern:
- C auris can spread between patients in healthcare facilities and cause outbreaks. In this way, it appears to behave much like some multidrug-resistant bacteria (eg, methicillin-resistant Staphylococcus aureus or Acinetobacter). Using contact precautions to prevent transmission may sound strange for Candida, but for C auris, they are a key part of the control strategy.
- C auris can colonize a patient’s skin for months or longer. It can be readily detected by culturing swabs of a colonized patient’s axilla, groin, or other body sites. In light of this, use of contact precautions, as well as strict attention to hand hygiene, are critical elements in controlling spread. CDC is also working with partners to better understand the role of topical agents to prevent spread by reducing colonization.
- This hardy yeast can live on surfaces for a month or more, and preliminary testing suggests that quaternary ammonium compounds commonly used for healthcare disinfection may not be sufficiently effective against C auris. Until further testing is available, CDC recommends that healthcare facilities meticulously perform daily and terminal cleaning of rooms of patients who were infected or colonized with C auris with an EPA-registered disinfectant that is effective against Clostridium difficile spores.
- C auris is quickly becoming more common. In some international healthcare facilities, it has gone from an unknown pathogen to a cause of 40% of invasive Candida infections within a few years. We need to act now to prevent this from happening in the United States.
- C auris is often multidrug resistant. Some strains have been resistant to all three major antifungal classes, including echinocandins, the first-line treatment for Candida infections.
- C auris has reportedly never been isolated from the natural environment, and it does not seem to have been a common colonizer of humans before 2009. More research is needed to understand where in the environment C auris lives and why it began affecting humans only recently.
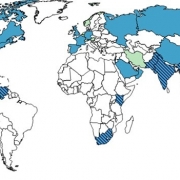
We are here – it is now that this multidrug resistant yeast is making its way into U.S. hospitals, with the CDC withholding information as to which hospitals are infected. The list of states reporting infestations is growing rapidly.
Read more on C. auris in the News. To read the entire article, click here.

 www.moldfreeliving.com
www.moldfreeliving.com 
 ©CDC.gov
©CDC.gov 



