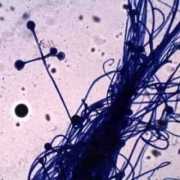
Candida Auris in the News
How to Confront a “Super Fungus” In An Increasingly Pathogen-Friendly World; reprinted by permission from www.moldfreeliving.com
Part One
From time to time, I try to use this blog as an opportunity to introduce and discuss the latest news topics concerning mold/fungus and human health that come onto the scene and temporarily dominate mainstream media platforms. These stories seem to pop-up overnight, consume headlines and social media feeds, and then disappear without warning or explanation, leaving all of us wondering if we still need to be concerned and vigilant. This is going to be one of those posts, because it is important to me to formally address the news of the “recently-discovered,” rapidly-emerging fungal pathogen, or “Super Fungus,” Candida auris.
Before I get into the details, I want to be clear as to why I decided to write about Candida auris when the topic has already been covered ad nauseam: It is my opinion that most current stories on Candida auris generate a climate of increased fear and confusion surrounding how and why the pathogen spreads, our inability to eliminate it with standard antifungal drugs and treatment, and the high fatality rates of those infected.
And while, those are definitely some of the hard facts about this fungus, Candida and other fungal infections have been around for centuries causing sickness and high mortality rates for systemic infection, but for some reason, just haven’t been given the focus, the importance, or the same “billing” as their bacterial and viral counterparts.
This has been especially true in the medical community. For example, just think about how many times you have walked out of a doctor’s office with a prescription for a broad-spectrum antibiotic. Did they take a culture and identify the specific pathogen before writing the prescription? On the other hand, how many times has a doctor mentioned the possibility of fungal source when you have been sick or has prescribed an antifungal? Not many, right?
Thus, I thought it might be helpful for me clear things up and to demystify Candida auris by focusing only on information that is evidence- and scientific-study based, so that I can bring you an easy-to-digest, and hopefully relatable take on the story. I also believe that when anything fungal is causing acute sickness to humans, especially at the magnitude of Candida auris, I would be missing the mark not to discuss some basic connections between the emergence of an increasingly virulent yeast and why we are becoming so vulnerable to it.
What is Candida auris?
If you Google “Candida auris,” you will find a multitude of stories and recently-published articles from various news outlets and the Centers for Disease Control (CDC) detailing the rather sudden (over the past 10 years) emergence and rapid spread of this potentially deadly and increasingly drug-resistant yeast. And, while various forms of Candida are nothing new to the medical world, heck, the yeast that causes diaper rash is part of our vernacular almost from birth, this particular yeast is different in that it is behaving more like a bacterium in its spread and ability to swiftly infect patients. While, for the most part, confined to immunocompromised patients in hospital or long-term care facilities, this “new” fungal invader has actually existed for thousands of years, but is only recently materializing as a growing medical threat worth a closer look.
To break things down as simplistically as I can, Candida auris (C. auris) is a species of fungus which grows as yeast (single-celled fungi). In people with healthy immune systems, cells called macrophages and neutrophils engulf these pathogens, nipping them in the bud. But when the immune system is weakened by disease or drugs, fungi can grow unchecked. Candida auris is one of the few species of the genus Candida which can cause candidiasis (fungal infection) in humans.
Many of the yeast infections with which we are most familiar are localized and can be treated. Less often, a fungal infection can enter the bloodstream and become systemic and fatal. Candidiasis infections are most often acquired in hospitals by patients with already weakened immune systems. Since C. auris is a pathogenic fungus that can cause invasive candidiasis (fungemia) in which the bloodstream, central nervous system, and internal organs are infected, it is especially dangerous to the most at-risk hospital patient population.
Candida auris was first described after it was isolated from the ear canal of a 70-year-old Japanese woman in 2009. Its mycology revealed it to be a fungus that could infect humans and, in severe cases, cause potentially fatal blood infections like those that we are seeing spread throughout certain chronically ill and immunosuppressed populations in hospital settings today—the most at risk populations being the elderly, diabetics, patients with venous catheters or feeding tubes, ICU patients, and those with other co-morbid conditions, especially those who have already been on high-dose antibiotics and/or antifungals. The factors of advanced age, suppressed immunity, and openings in the skin and mucous membranes seem to be what helps Candida auris (and most hospital-acquired fungal infections) gain access to the body.
Do I Need to Be Concerned About Being Infected?
While Candida auris doesn’t appear to pose eminent danger outside of hospitals and long-term care facilities yet (all reported cases have been confined to those settings and populations), understanding how and why it is spreading may be the best way to go about answering this question.
So far, the spread of Candida auris has been swift and broad. To date, the fungus has been reported and identified in more than 30 countries around the world, including the United States (the first reported case in 2013), Australia, India, Germany, Israel, Venezuela, and South Africa. But Candida auris has not been traceable in the same way most outbreaks tend to be, with an identifiable host, epicenter and a circular projection of cases spanning and growing all around it.
Rather, Candida auris, from an epidemiologic perspective, seems to be evolving separately and independently on each continent. In other words, the fungus is changing, adapting, and spreading within each different environment, independent of its source or host. For example, strains of the fungus in one country have different anti-fungal resistance than those in another, with some strains even developing resistance during drug usage. Doctors usually do not know which exact drugs will be effective until a patient begins treatment.
This also makes prevention and identification of new cases challenging, because:
- Specific testing mechanisms are required to properly diagnose an infection and not all hospitals have those capabilities or enough experience with the pathogen yet to have to have the foresight to do so, making misidentification frequent and problematic for swift intervention;
- Most patients that acquire invasive Candida auris also have other significant health issues, so the symptoms are not always glaringly apparent until the infection has spread systemically in the blood or progressed to a very serious state;
- And, when treatment with antifungal drugs begins, the patient has to be frequently checked and evaluated for progress, since no one drug seems to be effective for most patients.
This concept of a fungus that is genetically evolving may be difficult to fully grasp, especially if you, like me, are not very scientifically inclined. But, this evolutionary divergence of different strains of the same pathogen that are all developing similar antifungal resistance is what makes C. auris both fascinating and scary. This is because, it shines a light on the fact that both our bodies and our environments are becoming more inviting hosts to pathogens and toxins.
And, while Candida auris may be a microcosm of this issue, it brings to the forefront that there is a misunderstanding and disparate level of education in the medical community when it comes to identifying and treating fungus as a pathogen and threat.
In other words, while the medical focus has been on bacteria and viruses, fungi have materialized as formidable dangers in many forms. Unfortunately, this fact also makes most doctors and healthcare facilities ill-prepared to defend against them. When you recognize this and also acknowledge that every single one of us or someone whom we love will likely have to be a patient in a hospital for some reason, at some point in our lives, knowing that Candida auris could be present and could possibly cause significant infection and illness is a concerning proposition.
Why is Candida auris So Difficult to Get Rid Of?
The answer seems to circle back to how the fungus is behaving. According to Dr. Tom Chiller, chief of the CDC’s Mycotic Diseases Branch, “It’s a yeast that’s acting like bacteria.”
Meaning, from an infectious disease perspective, that Candida auris is doing what “germs” do, not what “fungus” is assumed to do. To put it simply, Candida auris’s environmental resiliency combined with its antifungal resiliency makes it easy to spread, but difficult to kill.
- It is staying alive on surfaces and medical equipment despite traditional cleaning and disinfectant protocols.
- It is spreading directly from one person to another through contact.
- It is colonizing and living on skin surfaces of hosts without their knowledge and absent symptoms.
- And, it is developing and sustaining resistance to many tiers of antifungal drugs that are typically used to treat invasive fungal infections.
A Frontiers in Medicine article about Candida auris sums this idea up well. “Although C. auris does not share some of the virulence factors found in many Candida species, the non-aggregative phenotype, in conjunction with its biofilm-forming ability and innate resistance to antifungal agents, may help explain why it is so pathogenic and resilient on environmental surfaces despite disinfection.”
The Environmental Resiliency of Candida auris
C. auris’s ability to hang around in the environment for a lengthy period of time (14 days is cited) may also lead to its pathology against medications. Additionally, C. auris has been cultured from contaminated bedding for up to 7 days. The persistence of this pathogen on environmental surfaces presents opportunities to colonize or infect hospitalized patients and healthcare workers. There is some evidence that skin colonization of C. auris can persist for weeks to months as well–this is similar to other yeasts. In turn, the transfer of this pathogen from colonized patients and healthcare workers also presents further opportunities for it to contaminate other environmental surfaces.
Once on surfaces, rather than becoming inert, Candida auris retains its ability to infect, as it is able to form biofilm (a protective layer or covering that is difficult to penetrate) with the other microbes present to protect itself. This has made cleaning the rooms of colonized or infected patients extremely difficult. This is obviously a very concerning aspect of C. auris and is getting further attention and study by the CDC as they seek to stop its spread.
To date, the CDC has found the best lines of physical defense to be stringent hand-washing and sanitizing protocols, isolating affected patients in separate rooms with posted warnings and infection protocols strictly adhered to, and using cleaning and disinfecting protocols in line with those used for Clostridium Difficile (an highly infectious and antibiotic resistant bacterium) in the rooms of affected patients both during their hospital stay and to clean their rooms after discharge. I will add that these advised cleaning products are mostly chlorine-based (not always the most effective chemical against fungus, as it does not address hyphae or biofilm).
As of now, from what I can see, little to no research has been done on naturally-derived cleaning products that have been proven effective against other fungi and mold as alternatives to the standard and more toxic chlorine and oxidizing products.
The Anti-Fungal Resiliency of Candida auris
Once a patient is infected, treatment can become especially difficult, because many prescription antifungals are ineffective against C. auris. For example, in a paper published on an epidemiological study of the C. auris cases in NY, in the first 51 clinical cases, all but one had C. auris strains that were resistant to fluconazole. One quarter of those cases were resistant to both fluconazole and amphotericin B. Since there are not that many classes of antifungal drugs, the fact that C. auris already has beaten the first line of defense is worrisome.
As the fungus is studied more and scientists are able to understand more about how and why it is adapting, new combinations of antifungals from different categories are being tried and some antifungals are even being given to some of the most at-risk patients preemptively to thwart infection. It is still yet to be determined whether or not these actions will be successful.
There is also little to no adoption in clinical settings of attempts to combine 2 antifungals which are structurally different in order to stop drug resistance during treatment. In addition, there are many natural herbals that, in combination with prescription antifungals, may work well, especially as preemptive therapy, like Oregano, caprylic acid, cinnamon, and pau d’arco. These herbals do not foster anti-fungal resistance either the way that prescription drugs do.
Unfortunately when a potentially fatal pathogen rears its ugly head, there are not many doctors or hospitals who would want to “try” such remedies to see what works. I can’t say I find fault with that, but this certainly identifies another possible line of defense that needs to be investigated further.
Making Additional “Fungal” Connections
Worth noting is also the evidence-based speculation about the new prevalence of C. auris having something to do with the use of azole anitfungals in the world’s food supply. These antifungals, when sprayed on produce, can create antifungal resistance both on the foods and in within the bodies of those ingesting them. This theory makes sense of the pathogen’s early ability to withstand even some of the most potent antifungal pharmaceuticals available, because, with this line of thought, C. auris has been adapting within our environment for a long time, so that now, as it surfaces, it is already extremely virulent.
Another interesting take on a possible pathophysiologic mechanism of the spread of pathogenic yeast—that you will NOT find elsewhere in the news, by the way—is that the typical “sick person” diet and the generic hospital diet are both high in carbs and sugar. Hospital IV’s also contain dextrose (sugar). Candida has a sugar receptor on the cell wall that causes it to change its physical shape from a harmless “yeast” form to an invasive hyphal form. Hyphae are like tentacles or roots that can grow down into tissue. They are often 3 feet long, microscopic and invade tissues to seek more sugar. The hyphal form of Candida is more drug resistant. You cannot kill it in the presence of sugar.
Therefore, with continual exposure to sugar, a patient is feeding the yeast, despite using antifungals to kill it. Further, environment plays a part in fostering yeast in the body, because all fungi have the same cell wall structure, so if a patient has been breathing fungal air and mycotoxins, they are already reacting to their own gut Candida which can be a tremendous inflammatory reaction that cripples the immune defense system. This both predisposes a person to infection and already gives yeast a foothold in their bodies.
Written by Catherine at www.moldfreeliving.com. To read the entire article, click here.

 www.moldfreeliving.com
www.moldfreeliving.com